Buh bye, pap smear!
Because I enjoy reading pap smears as much as the next pathologist, I was saddened to read about the pending demise of the beloved cervical cytology specimen. About a week ago, an FDA advisory panel recommended use of a DNA-based HPV test for cervical screening. The Roche Cobas 4800 (http://www.roche.com/media/media_releases/med-cor-2014-03-13.htm) is the recommended testing platform that could dry up the revenue stream for many cytology laboratories.
Cyto-histo correlations and colposcopy conferences could become a thing of the past. Prominent cytopathologists might lose the ability to take junkets to suburban Maryland in order to consense about diagnostic criteria. The moral quandary over whether to continue looking at an equivocal pap smear or just call it “ASCUS” might just disappear!
All joking aside, this move actually might be really good for female patients who are subject to repeated unnecessary exams and needless worry. And the resulting change in clinical practice will challenge the pathology community to continue to adapt in order to survive and to maintain relevance. How many cyto techs and cytopathologists will be replaced by a Roche machine? We’ll find out soon enough.
Dr. Daniel Cruser is a practicing pathologist in New York.
What is next digital slides versus analog slides?
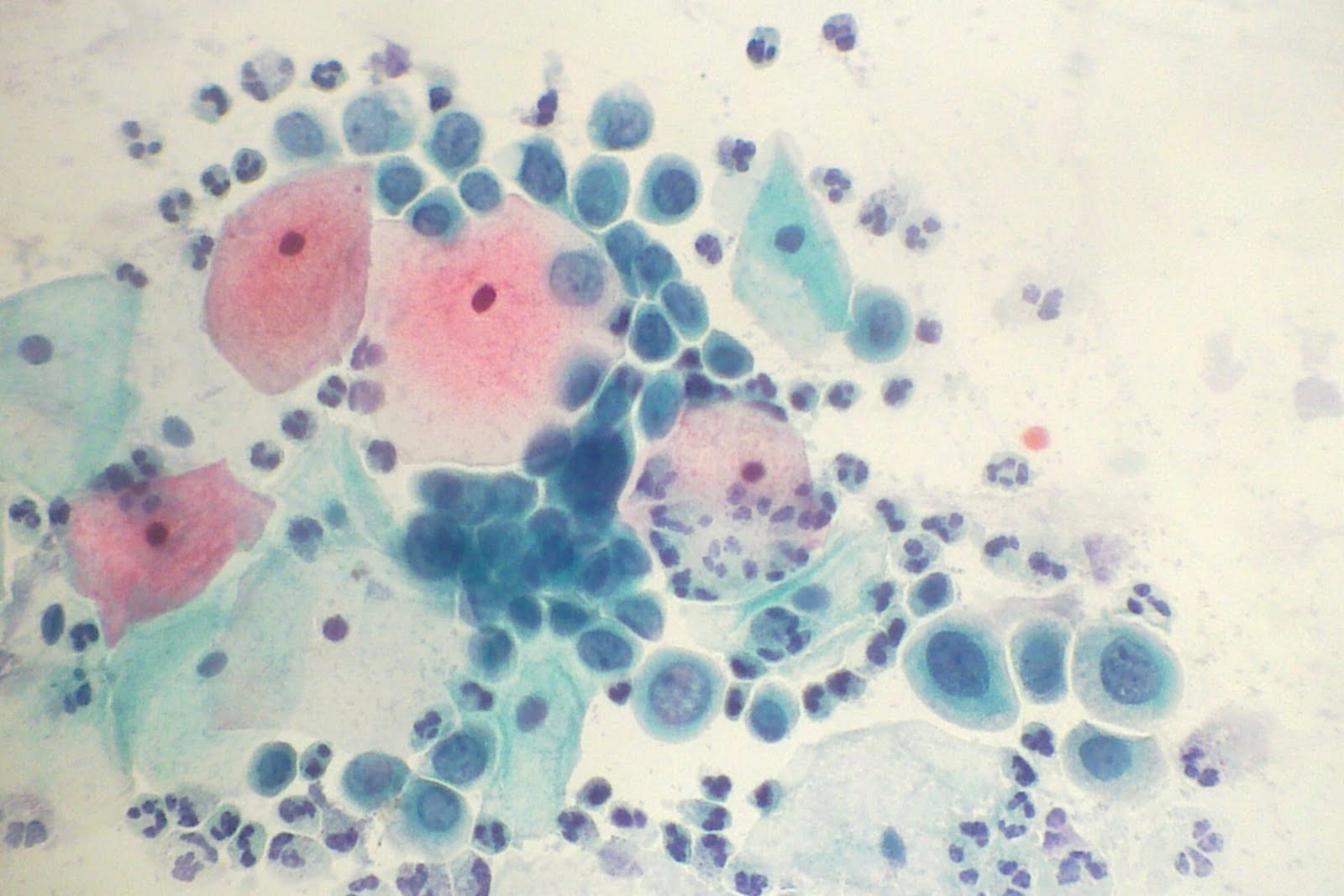 The cervical pap smear has served humanity well as the most effective cancer screening test in history. Newer technologies that build upon lessons learned from the former technology are a never ending goal for medicine and healthcare. If you can replace subjectivity with objectivity and manual processes with automation shouldn’t we all consider better, faster, more sensitive/specific tests to arrive at the right diagnosis? For those of us who read first conventional and later liquid-based pap smears and are fans of Dr. Papanicolaou, perhaps some crocodile tears will be shed.
The cervical pap smear has served humanity well as the most effective cancer screening test in history. Newer technologies that build upon lessons learned from the former technology are a never ending goal for medicine and healthcare. If you can replace subjectivity with objectivity and manual processes with automation shouldn’t we all consider better, faster, more sensitive/specific tests to arrive at the right diagnosis? For those of us who read first conventional and later liquid-based pap smears and are fans of Dr. Papanicolaou, perhaps some crocodile tears will be shed.
About the cobs HPV Test and cobas 4800 System
Clinically validated by the landmark ATHENA trial, the cobas HPV Test is the only FDA-approved HPV assay that provides specific genotyping information for HPV 16 and 18, the highest-risk types, while simultaneously reporting the 12 other high-risk HPV types as a pooled result, all in one run, from one patient sample.
The cobas HPV Test received FDA approval in April 2011 for screening patients age 21 and older with abnormal cervical cytology results and for use adjunctively with normal cervical cytology in women ages 30 and over to assess the presence or absence of high-risk HPV genotypes. Roche submitted their Premarket Approval (PMA) supplement for the cervical cancer primary screening indication with the FDA in June 2013. The filing includes 3-year follow-up data from the ATHENA study, Roche’s landmark U.S.-based registration trial. ATHENA enrolled more than 47,000 women who were screened for cervical disease and an impact analysis of screening algorithms was performed based on these data.
The test is performed on the cobas 4800 System, which offers true walk-away automation of nucleic acid purification, PCR (polymerase chain reaction) set-up and real-time PCR amplification and detection to help laboratories achieve maximum efficiency. The system also runs the cobas CT/NG Test (chlamydia/gonorrhea), the cobas BRAF V600 Mutation Test and the cobas EGFR Mutation Test.