While You Were Sleeping – Do You Know Where Your Specimen Is?
What really happens to your surgical specimen?
It is one of the most frightening events in a person’s life… an unusual lump that needs to come out. You visit your primary care physician. He refers you to a “specialist” who will remove your unusual growth while you are under anesthesia. What happens to that piece of you once it is out of your body? Great question! The process might vary depending on what type of tissue it is. Why? There are only standards in place for ONE type of tissue, breast tissue.
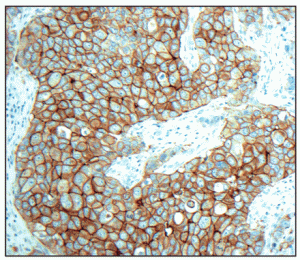 Why are there standards for breast tissue? In 1998 a drug was developed to target a very specific type of breast cancer, HER2 positive breast cancer. A companion diagnostic test was developed to identify those patients with this very specific type of breast cancer to qualify patients for the targeted therapy. Variations in pre-analytic factors, testing and interpretation of the test results muddied the water for qualifying these patients for this potentially life-saving therapy. The College of American Pathologists (CAP) and the American Society of Clinical Oncology (ASCO) recognized the stricter protocols must be enforced to improve the companion diagnostic qualification.
Why are there standards for breast tissue? In 1998 a drug was developed to target a very specific type of breast cancer, HER2 positive breast cancer. A companion diagnostic test was developed to identify those patients with this very specific type of breast cancer to qualify patients for the targeted therapy. Variations in pre-analytic factors, testing and interpretation of the test results muddied the water for qualifying these patients for this potentially life-saving therapy. The College of American Pathologists (CAP) and the American Society of Clinical Oncology (ASCO) recognized the stricter protocols must be enforced to improve the companion diagnostic qualification.
What this means for a breast tissue specimen is that every process from the time blood supply is cut off to the tissue (warm ischemia) to the time the tissue is removed from the body (cold ischemia) to the time the tissue is placed in fixative (10% Neutral Buffered Formalin) is closely monitored and recorded. This information is captured on the patient’s surgical report. If a specimen is greater than 2 mm in diameter, the specimen must be further dissected by a pathologist or a pathologists’ assistant (PA) and placed in fixative/10%NBF within one hour of removal from the body. This process ensures that the tissue remains viable and morphologically intact for additional routine and special testing done by the pathology laboratory.
Why are these practices important? If there is a potentially life-saving therapy for your diagnosis, proper testing is the only way to know for sure. The specimen is only as good for testing as the way it is handled prior to testing.
Your unusual lump was a living, growing part of you. Once you cut off the blood supply, the tissues begin to change. If left out, the cells will break down, the DNA, the proteins may become less viable for necessary testing.
Back to your tissue… Not breast tissue? You better check out the hospital or doctor’s office performing the procedure (before you go to sleep). The very first question on your mind at this point should be “Does this facility have pathology services onsite?” If not, if specimens are processed centrally, when will they be picked up and “accessioned” and “grossed”?
Why is that a big deal? There are no regulations for any other tissue types than breast. Sure, there are recommendations. My mom recommended that I eat my vegetables and wear my bicycle helmet and never kiss on the first date. Didn’t happen. Recommendations are just that… suggestions, not rules with penalties for disobedience. Those facilities with breast tissue may get cited during CAP inspections if laboratories are not following the guidelines that they set forth.
What is your lump? How big is it? If it’s bigger than a nickel and a pathologist or PA doesn’t do a gross dissection on it within that magical one hour time frame from when it came out of you, it will start to break down chemically. This will destroy the proteins, the DNA, the tissue morphology. These are the things that help the pathologist diagnose your condition that will drive your treatment options. The worse case scenario is that the facility that did your surgical procedure and took out your lump with minimal or no required fixative for your tissue specimen to transport it down the crowded highway to the pathology lab to grossly dissect it. So how far away is that lab? How big is your lump?
Some hospitals are cutting pathology services onsite to consolidate efforts, therefore, saving money. Your lump may be spending several hours in the back of a car in a bucket, ideally with a 20:1 fixative to tissue ratio. Small (<2mm in diameter or smaller than a nickel) specimens will fix very nicely as they travel down that lonesome highway. Anything larger may degrade without appropriate fixation. You see, fixation is a very slow process. 10% NBF only penetrates your lump at 1mm/hour and will only fix tissue at a rate of 2-3 mm in 24 hours. Your tissue will start to degrade after an hour. If you have a lump the size of a golf ball, only the outer most surface will be worth looking at. Last time I checked, surgeons like to remove margins around the lump just in case it is something bad. So the “bad stuff” in the middle may not be as well fixed. Guess what? You can’t undo the damage to the DNA and proteins. This may hamper further testing for HER2 as well as ER and PR if the tissue is not fixed appropriately in the appropriate amount of 10% NBF.
In conclusion, do your homework. Ask where the facility sends their pathology. Is there a pathology lab onsite or is it 30 miles away? Is it staffed 24/7. If you have a procedure at 3pm on Friday, is it going to sit in formalin over the weekend before someone grossly dissects it so that the surfaces can adequately be exposed to fixative? You need to ask these questions and advocate for your tissue, your lump, your cancer. Find an appropriate place for it to be handled properly so that you may get an accurate diagnosis and explore all the treatment options available to you.

































