Mammograms Tied to Over Diagnosis of Breast Cancer
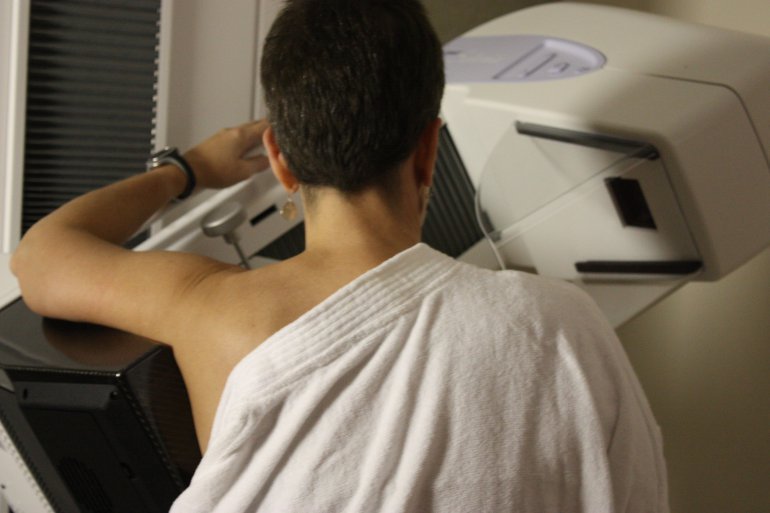 This kind of news seems to come up with some regular frequency – “To screen or not to screen, that is the question”. This Danish study recently reported in the Annals of Internal Medicine found that screening was not associated with a lower incidence of advanced tumors and argues that slow-growing, clinically less aggressive tumors may be over diagnosed leading to unnecessary treatment and social issues that come with having a malignant diagnosis.
This kind of news seems to come up with some regular frequency – “To screen or not to screen, that is the question”. This Danish study recently reported in the Annals of Internal Medicine found that screening was not associated with a lower incidence of advanced tumors and argues that slow-growing, clinically less aggressive tumors may be over diagnosed leading to unnecessary treatment and social issues that come with having a malignant diagnosis.
According to Dr. Otis Brawley, Chief Medical Officer of the American Cancer Society who provided a phone interview for the below story and wrote an accompanying editorial to the study says it is not time to change the screening guidelines just yet. Dr. Brawley contends that “If it’s small and slow-growing, I think all breast cancers ought to be treated.”
Without knowing the best clinical practice right now we may have to over screen and over diagnose and over treat at the expense of detecting more tumors that are not as advanced while still not increasing ability to detect those tumors that are more advanced with active screening programs. The authors of the study do point out results may be different today with improved mammography techniques but I think society is still confounded with what might represent too much screening such as with breast cancer screening programs.
Perhaps increased molecular techniques performed on tissue obtained from biopsies in women with abnormal mammograms who follow the guidelines will eliminate unnecessary surgery, radiation and chemotherapy in the future…
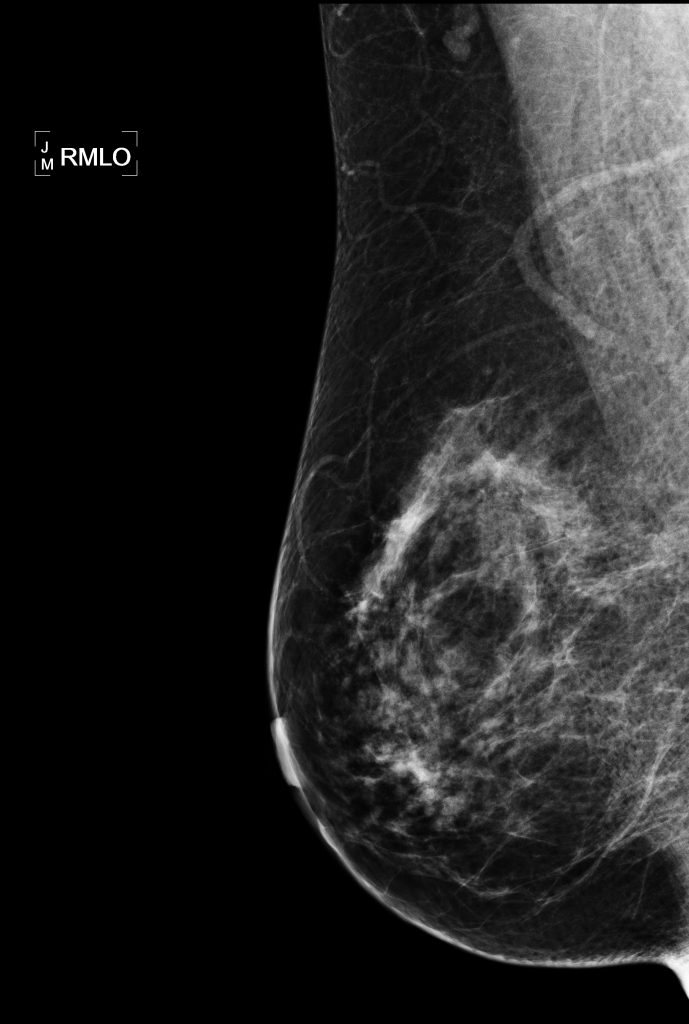 (Reuters Health) – Widespread breast cancer screening may catch more small, slow-growing tumors that are unlikely to be fatal without curbing the diagnosis of advanced cancer cases, a Danish study suggests.
(Reuters Health) – Widespread breast cancer screening may catch more small, slow-growing tumors that are unlikely to be fatal without curbing the diagnosis of advanced cancer cases, a Danish study suggests.
Diagnosis rates for ductal carcinoma in situ (DCIS) have surged in recent years as more women get screening mammograms.
The current study offers fresh evidence linking routine screening to over-diagnosis of non-aggressive tumors because it compares outcomes over a single time period in two regions of Denmark – one that offered biennial mammography for women aged 50 to 69 and one that didn’t.
“Over diagnosis means that healthy women get unnecessary breast cancer diagnoses,” said lead study author Dr. Karsten Juhl Jorgensen, of the Nordic Cochrane Center and Rigshospitalet in Copenhagen.
“A breast cancer diagnosis is a life-changing event for the woman and her family, with substantial implications for their quality of life,” Jorgensen added by email. “It also leads to overtreatment with surgery, radiotherapy and sometimes chemotherapy – we know these treatments have serious, sometimes lethal, consequences.”
The goal of mammograms is to detect tumors before they can be felt in a physical breast exam, catching cancer sooner when it’s easier to treat. Ideally, this should mean fewer women are diagnosed when tumors are bigger, rapidly growing, and harder to attack.
To see how well mammograms achieve this ideal, researchers examined data on more than 1.4 million Danish women aged 35 to 84 from 1980 to 2010.
Organized breast cancer screening programs began in Copenhagen in 1991, Funen in 1993 and Frederiksberg in 1994 – altogether covering about 20 percent of the population. Other regions gradually introduced screening starting in 2007.
Screening wasn’t associated with a lower incidence of advanced tumors, researchers report in the Annals of Internal Medicine, January 9.
This raises doubts about whether mammography reduces breast cancer deaths, the researchers conclude.
In addition, researchers estimate that as many as one in three breast tumors diagnosed in women who got mammograms would never have caused a noticeable health problem or led to death – and are therefore examples of over diagnosis.
One limitation of the study is that because mammography has improved since this study began in 1980, women might get different results today, the authors note.
While the study adds compelling evidence that routine mammograms carry a risk of over diagnosis, that doesn’t mean it’s time for screening guidelines to change, Dr. Otis Brawley, chief medical officer of the American Cancer Society, said in a phone interview.
Under current U.S. guidelines, mammograms should be optional for women aged 40 to 44, then done annually from 45 to 54. Women 55 and older should switch to mammograms every two years, continuing as long as they are in good health with a life expectancy of at least a decade.
“This isn’t about saying don’t get a mammogram, this is about using it most effectively to save the most lives,” said Brawley, who wrote an editorial accompanying the study.
Beyond screening, there are other preventive measures women shouldn’t overlook like eating well, getting plenty of exercise, and maintaining a healthy weight.
In the future, it may be possible to use screening results to pinpoint women who might be candidates for “watchful waiting,” the close follow-up without treatment that’s common for many men with early-stage prostate cancer, Brawley said.
“We aren’t ready for that because we don’t know what watchful waiting looks like for breast cancer yet,” Brawley said.
So for now, that means accepting that over diagnosis and screening go hand in hand, along with the potential for some women to get unnecessary treatment.
“If it’s small and slow-growing, I think all breast cancers ought to be treated,” Brawley added.
Source: Journal of Clinical Pathways and Annals of Internal Medicine

































